How does our body react to stress?
Is it really any coincidence that London seems to be full of stressed people suffering with digestive problems and lack of sleep?
The pace of life, the volume of people and the daily demands in a busy city are a good example of what happens when we are exposed to constant stressors.
In actual fact, it makes no difference what is causing the stress, the real problem is the chain reaction of stress hormones released in the body as it physically prepares to fight against, or flee from any perceived threat:
- Blood is diverted to the brain, heart, lungs and muscles, which will need to work well to get you out of danger
- The heart beat speeds up to pump blood more effectively round the body to these areas
- Blood is diverted away from the digestive tract, as stopping for a picnic shouldn’t really be on the agenda when there’s a life and death situation going on
- Breathing speeds up to get oxygen supplies to the muscles as quickly as possible
- Sweat levels go up to stop the body from overheating
- Blood sugar levels go up dramatically so that glucose is available to feed the brain and muscles
- Blood vessels constrict.
The overall effect is higher blood pressure, digestive problems, anxiety, tense muscles and palpitations. If your body is flooded with stress hormones continuously, these symptoms worsen.
What happens to the digestive system when we are stressed?
Under normal circumstances our digestive system should be able to go about its daily task of mixing, contracting and absorbing, to help break down our food and begin extracting the nutrients and vitamins that we require for good health.
However, when stress hormones are flooding our body, our digestive system effectively shuts down, causing our digestive muscles to contract more or less frequently, our gastric secretions and stomach acid levels to increase or decrease and our healthy gut bacteria to change composition.
At the very time we need to slow down, breathe, rest and digest, we bolt our food, eat on the run and make life even harder on our digestion.
image: https://experiencelife.com/article/tangled-up-in-food/

What are the digestive symptoms we are likely to experience?
- Fewer digestive secretions are made to help us digest food (causing more wind, bloating and nausea)
- Stomach acid levels can increase (causing acid reflux, pain and inflammation)
- The digestive contractions can increase or decrease (diarrhoea, constipation, spasm, etc.)
These symptoms also leave us open to compromised immunity (with at least 70% of our immune cells in our gut), infection, and further impact on our mood.
The brain in the gut or Enteric Nervous System
The important link between the gut and the brain also needs to be mentioned. We have all heard of 'gut feelings' or 'having butterflies' in certain situations.
This is thought to be due to the Enteric Nervous System (ENS) or the 'brain in the gut' linking digestive function to mood and vice versa. The ENS is two thin layers of more than 100 million nerve cells lining our gastrointestinal tract from oesophagus to rectum.
A highway of nerves runs directly from our actual brain to our digestive system, and messages flow in both directions between the two.
Did you know?
95 percent of the body's serotonin (a hormone that helps control mood, sleep, appetite) is found in the digestive system, not the brain.
The ENS may trigger big emotional shifts experienced by people coping with irritable bowel syndrome (IBS) and functional bowel problems such as constipation, diarrhoea, bloating, pain and stomach upset.
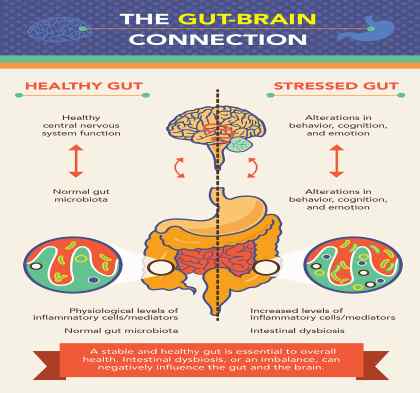
image: https://www.northwestpharmacy.com/healthperch/gut-health/
“For decades, researchers and doctors thought that anxiety and depression contributed to these problems. But our studies and others show that it may also be the other way around,” explains Jay Pasricha, M.D., director of the Johns Hopkins Center for Neurogastroenterology, whose research on the enteric nervous system has gained international attention. Researchers are finding evidence that irritation in the gastrointestinal system may send signals to the central nervous system (CNS) that trigger mood changes.
“These new findings may explain why a higher-than-normal percentage of people with IBS and functional bowel problems develop depression and anxiety,” Pasricha says. “That’s important, because up to 30 to 40 percent of the population has functional bowel problems at some point.”
How can we help ourselves?
If you notice any change in digestive function, do consult with your GP or healthcare provider. They will be able to ask certain questions and arrange any applicable tests to help determine the cause. If stress is considered to be the main culprit, addressing the source of the stress should naturally be a priority.
Talking therapies
'Talking therapies' which involve working with a qualified therapist to find better ways to deal with stress should not be underestimated. Methods such a CBT, which addresses intrusive and unwanted thought patterns can be particularly helpful, and have been shown to improve symptoms of irritable bowel syndrome by up to 70 percent in some people, over a period of a few months.
Listen to your gut
Given the link between the gut and the brain we can be wired to react to certain foods, and may feel better avoiding them. Have you ever felt tired, nauseous, or a little “fuzzy” after a meal? If so, your enteric nervous system may be reacting to something you ate. Pay attention to how you feel after eating. If it helps you to keep track, try writing a food diary for a few weeks or consult with a nutritional therapist. (www.bant.org.uk)
Balanced diet
The body is always working towards balance and this is a sensible way to approach what we eat. The digestive system appreciates a healthy, whole food, well-balanced diet. When under stress we may instinctively reach for extremes in sugar, fat, caffeine, alcohol and processed foods but this can just exacerbate the stress cycle and digestive dysfunction.
Eating mindfully
If our Sympathetic Nervous System (the part of nervous system in charge of 'fight or flight') has been in overdrive, we need to counterbalance the effects by switching on our Parasympathetic Nervous System (the part of the nervous system in charge of 'rest and digest').
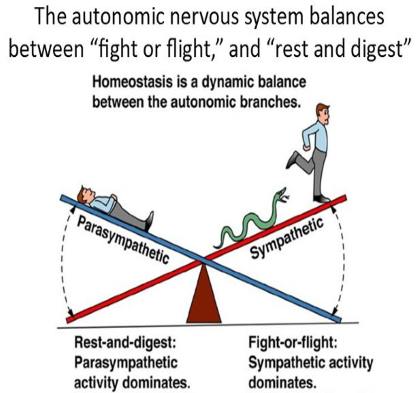
Copyright© 2007 Pearson Education, Inc, publishing as Benjamin Cummings
One of the ways we can do this is to aim for the experience of mindful eating rather than refuelling. In other words, rather than grabbing food and eating on the run, we endeavour to take time to sit down, relax and enjoy our food.
Chew, chew and chew some more
If we could only change one thing, my recommendation would be to chew, chew and chew some more. As our digestion expert Ali says, ‘Don’t bolt your food down. If it hardly touches the sides as it goes down, the chances are the digestive system won’t be ready for it and all sorts of mayhem will break out. Try chewing each mouthful 20 times for a while and surprise yourself with how much better your digestive tract feels.’
The process of chewing not only helps to break down food into digestible particles but also produces digestive enzymes through saliva. The more we chew, the easier on our stomach and small intestine and the better we are likely to digest, avoiding unpleasant symptoms.

image: https://www.fix.com/blog/mindfulness-techniques-to-reduce-stress/
Avoid drinking with meals
When we drink fluid with a meal we dilute our natural digestive enzymes and potentially wash down the food before it has been properly broken down. To maximise digestive potential, stick to drinking 20 or 30 minutes before or after a meal.
Exercise
Moderate exercise is one of the best ways to manage stress and maintain healthy digestion. Physical activity relieves tension and stimulates the release of those feel good chemicals called endorphins which naturally improve our mood.
According to studies a post-meal walk can speed up the rate at which food moves through the stomach as well as decreasing blood sugar and lowering cardiovascular risk.
Relaxation therapy
People who have stress-related digestive problems often benefit from relaxation therapies such as yoga, meditation, hypnosis, progressive muscle relaxation, and even soothing music. IBS sufferers have been found to experience a significant reduction in pain and bloating through practising these techniques.
Bowel Essence and Bitters
As an IBS sufferer, two of my favourite ways to tackle digestive dysfunction are flower essences and bitters.
I was introduced to Bowel Essence during a particularly stressful time in my life and was advised that this flower essence combination may help relieve emotionally triggered digestive issues. Its significant impact surprised me and, needless to say, it has been a constant companion ever since!
Bitter herbs were also a revelation to me in their ability to improve digestive function, assimilation and elimination. Anyone suffering with digestive issues can benefit from including bitter foods in the diet, such as chicory, dandelion root coffee, artichoke, watercress, rocket, etc.
A tincture of bitters such as Digestisan in a little water, 20 minutes or so before meals, can also be such a helpful formula for those needing the extra digestive support.